This topic is a very personal one for me as my son Wyatt has an AVSD, albeit a small balanced one. In fact, it was the discovery of his AVSD in utero that told us that he probably had a chromosomal disorder.
It is a terrifying thing to hear that your baby has a hole in his or her heart. If my son had been born as little as thirty years ago, his prognosis probably would not have been as good. I am lucky in a way, as I am a Registered Nurse and therefore have a little bit of knowledge in this area (and know how to readily access more). Many parents do not. It is my hope that by creating this piece, I will arm parents with a little knowledge and dispel some fear by giving you a no-nonsense, straightforward (yet not too technical) explanation of what the heck AVSD is and what it will mean for your family.
AVSD is a structural defect of the heart that affects multiple organ systems. It is very common, accounting for 5% of all congenital heart defects and 17% of heart abnormalities discovered in utero in the general population. 42 to 48% of children with Down Syndrome have a heart defect; 45% of these are AVSDs.
Mainly made of muscle and connective tissue, the heart itself is a complex organ, In order to understand what an AVSD is, it is important to understand the specific structures of the heart and how this affects blood flow to the entire body.
Blood Flow Through the Heart
The heart, essentially, is a pump that moves blood around the body. As the tissues of the body require the oxygen that we breathe, the heart provides the force needed to deliver the blood and its oxygen payload to the cells, then return the deoxygenated blood to the lungs to 'refuel' and pick up oxygen again. As with all mammals, humans have a heart that is highly specialized. The left side of the heart deals with oxygenated blood, the right, deoxygenated blood (blood that has delivered its oxygen). The wall dividing the right from the left side that travels the length of the heart is known as the septum (shown here in pink).
The heart is further divided by two sets of valves, creating, in essence, quadrants. The top two quadrants are referred to as atria, while the bottom two are referred to as ventricles. The right atrium and ventricle are separated by the tricuspid valve, while the left atrium and ventricle are divided by the mitral valve.
Deoxygenated blood is brought to the right side of the heart (from the rest of the body) via two large veins known as the superior and inferior vena cava. It is pumped to the right atrium, through the tricuspid valve to the right ventricle and then up and out through the pulmonary valve to the pulmonary arteries where it is taken to the lungs to receive oxygen. The blood returns to the heart through the pulmonary veins and enters the left atrium. It is then pumped through the mitral valve, then into the left ventricle where it passes through the aortic valve and into the aorta and out to the body. As the oxygenated blood in the left side of the heart has farther to go (ie: the entire body) than the right side (ie: to the lungs), the left atria and ventricle are of a higher pressure than the right, giving them more 'push' with each beat.
Click this link to view an animated representation of blood flow through a normal human heart*
AVSD and Blood Flow
An Atrioventricular Septal Defect is just as it sounds, really: it is a "hole" or a missing part of the septum of the heart, extending from the atria down to the ventricles. Instead of a mitral and tricuspid valve, there is a "shared" or common valve in the centre. An AVSD can be described as "complete", where the entire septum is missing, "intermediate", where the ventricular aspect is small and "partial". In reality, there are many different ways to describe an AVSD, based on what structures are altered; for our purposes we will continue to use these terms. In a partial AVSD, there are two distinct valves instead of a shared one although typically, they will not function as well as they should.
Since a piece of the partition is missing, the oxygenated and deoxygenated blood mix. As the left side of the heart is under higher pressure, the blood is pushed to the right side of the heart and forces more blood than normal into the pulmonary veins and into the lungs. The mixing of the blood delivers less oxygen to the body, causing the heart to work harder, which in turn forces more blood into the lungs.
In a "balanced" AVSD, the pressures in the heart stabilize to a "medium" pressure area; although the blood from both sides mixes somewhat, it is not as dramatic as it is not being actively pushed from one side of the heart to the other due to a pressure differential. As a result, less blood is pushed into the lungs.
Click this link to view an animated representation of blood flow with an AVSD*
Diagnosis of an AVSD
AVSD can be diagnosed in utero by an ultrasound (a fetal echocardiogram). In a normal heart, the junction of the two valves, plus the septum make a distinctive cross formation. With an AVSD, the cross formation is incomplete.
AVSD Symptoms
Initially, an AVSD may be treated with diuretics (such as Lasix) and ACE inhibitors (such as Ramipril) and antiarrhythmics (such as digoxin) to alleviate symptoms and give the patient some time to stabilize and/or grow before surgery.
Although some rare instances do close on their own, the vast majority of AVSDs require some form of surgical intervention (that varies, depending on the type and structures involved). Most often, complete AVSDs are repaired between 3-6 months of age and partial/intermediate taking place between 6-18 months. Once again, the severity, placement and structures involved dictate the precise procedure. Smaller "holes" may just require closing, where larger areas need to be "patched". Although this used to mean hospital stays of weeks at a time, most children are discharged home within just over a week of their surgery (the stay for complete AVSD repair is longer as it is more involved).
The survival rate for AVSD is also dependent on type, however all range between a 97-99% success rate. Follow up surgery may be required years later to tune up leaky valves (specifically the mitral valve). Anticoagulants may be prescribed if the valves become too leaky to prevent blood clots from forming. In the event that the electrical conduction of the heart becomes damaged, a pacemaker may have to be surgically installed. Later in life, a condition known as Sub-Aortic Stenosis can occur, where a blockage forms below the aortic valve and requires surgery to repair. Endocarditis can develop and any invasive procedures (such as dental cleanings, surgery, piercing and tattooing) will require antibiotics prior to prevent large amounts of bacteria from entering the bloodstream.
In Conclusion...
The diagnosis of an AVSD is no longer a death sentence. With recent advances in medicine, the management and repair of AVSDs has become almost routine. Although it remains a significant life event for you and your family, your child's diagnosis need not overwhelm every aspect of daily life. The vast majority of people (regardless of chromosome count) that have an AVSD repaired, go on to live happy, healthy, productive lives. It is difficult to learn that your child has a genetic disorder, of this I can attest first hand. Hearing that your child has issues with his or her heart can be even more frightening. However, with a little education and insight, this aspect of your child's health need not be devastating to you or your way of life.
It is a terrifying thing to hear that your baby has a hole in his or her heart. If my son had been born as little as thirty years ago, his prognosis probably would not have been as good. I am lucky in a way, as I am a Registered Nurse and therefore have a little bit of knowledge in this area (and know how to readily access more). Many parents do not. It is my hope that by creating this piece, I will arm parents with a little knowledge and dispel some fear by giving you a no-nonsense, straightforward (yet not too technical) explanation of what the heck AVSD is and what it will mean for your family.
AVSD is a structural defect of the heart that affects multiple organ systems. It is very common, accounting for 5% of all congenital heart defects and 17% of heart abnormalities discovered in utero in the general population. 42 to 48% of children with Down Syndrome have a heart defect; 45% of these are AVSDs.
Mainly made of muscle and connective tissue, the heart itself is a complex organ, In order to understand what an AVSD is, it is important to understand the specific structures of the heart and how this affects blood flow to the entire body.
Blood Flow Through the Heart
The heart, essentially, is a pump that moves blood around the body. As the tissues of the body require the oxygen that we breathe, the heart provides the force needed to deliver the blood and its oxygen payload to the cells, then return the deoxygenated blood to the lungs to 'refuel' and pick up oxygen again. As with all mammals, humans have a heart that is highly specialized. The left side of the heart deals with oxygenated blood, the right, deoxygenated blood (blood that has delivered its oxygen). The wall dividing the right from the left side that travels the length of the heart is known as the septum (shown here in pink).
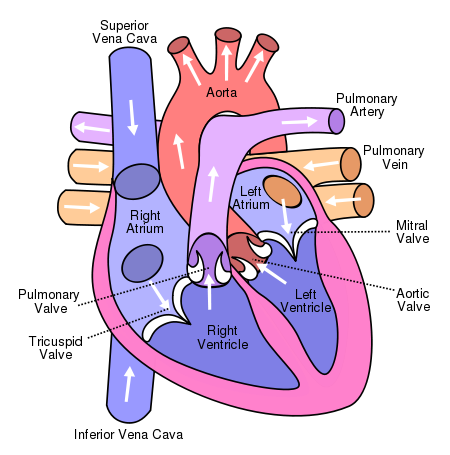 |
| Diagram of the human heart, by Wapcaplet, Creative Commons. |
The heart is further divided by two sets of valves, creating, in essence, quadrants. The top two quadrants are referred to as atria, while the bottom two are referred to as ventricles. The right atrium and ventricle are separated by the tricuspid valve, while the left atrium and ventricle are divided by the mitral valve.
Deoxygenated blood is brought to the right side of the heart (from the rest of the body) via two large veins known as the superior and inferior vena cava. It is pumped to the right atrium, through the tricuspid valve to the right ventricle and then up and out through the pulmonary valve to the pulmonary arteries where it is taken to the lungs to receive oxygen. The blood returns to the heart through the pulmonary veins and enters the left atrium. It is then pumped through the mitral valve, then into the left ventricle where it passes through the aortic valve and into the aorta and out to the body. As the oxygenated blood in the left side of the heart has farther to go (ie: the entire body) than the right side (ie: to the lungs), the left atria and ventricle are of a higher pressure than the right, giving them more 'push' with each beat.
Click this link to view an animated representation of blood flow through a normal human heart*
AVSD and Blood Flow
An Atrioventricular Septal Defect is just as it sounds, really: it is a "hole" or a missing part of the septum of the heart, extending from the atria down to the ventricles. Instead of a mitral and tricuspid valve, there is a "shared" or common valve in the centre. An AVSD can be described as "complete", where the entire septum is missing, "intermediate", where the ventricular aspect is small and "partial". In reality, there are many different ways to describe an AVSD, based on what structures are altered; for our purposes we will continue to use these terms. In a partial AVSD, there are two distinct valves instead of a shared one although typically, they will not function as well as they should.
Since a piece of the partition is missing, the oxygenated and deoxygenated blood mix. As the left side of the heart is under higher pressure, the blood is pushed to the right side of the heart and forces more blood than normal into the pulmonary veins and into the lungs. The mixing of the blood delivers less oxygen to the body, causing the heart to work harder, which in turn forces more blood into the lungs.
In a "balanced" AVSD, the pressures in the heart stabilize to a "medium" pressure area; although the blood from both sides mixes somewhat, it is not as dramatic as it is not being actively pushed from one side of the heart to the other due to a pressure differential. As a result, less blood is pushed into the lungs.
Click this link to view an animated representation of blood flow with an AVSD*
Diagnosis of an AVSD
AVSD can be diagnosed in utero by an ultrasound (a fetal echocardiogram). In a normal heart, the junction of the two valves, plus the septum make a distinctive cross formation. With an AVSD, the cross formation is incomplete.
|
|
| (Images courtesy of Ultrasound Image Gallery) |
 |
| ECG with AVSD (Image courtesy of Paediatric ECG |
After the child is born, an AVSD can be heard (auscultated) through a stethoscope as a heart murmur. An electrocardiogram (ECG or EKG) will show a distinct pattern. An oxygen saturation monitor would indicate when the blood had a lower than normal level of oxygen. A chest X-ray would show the size, position and shape of the heart, which would indicate any enlargement or megality, hypoplasia, etc. The infant's temperature, pulse rate, blood pressure and respiration rate is also used for assessment purposes, as is specific blood work.
AVSD Symptoms
Infants with an AVSD generally start to show symptoms a few months after birth. Initially they will have problems feeding and will tire easily. The child will sweat, will breathe harder and faster and grow slowly and/or lose weight. They may be blue and may have frequent chest infections. As the blood is forced into the lungs and the body does not receive the oxygen it needs, typically pulmonary edema and congestive heart failure ensue.
Occasionally this does not occur in an infant with a complete AVSD; instead a condition called Pulmonary Vascular Resistance (PVR) develops. In this, the smaller arteries of the lungs are constricted by the surrounding muscles to prevent them from being congested with the extra blood by the higher pressures of an AVSD. Due to this, many of the symptoms of congestive heart failure are prevented, including decreasing the amount of blood pushed (or "shunted") from the left to the right side of the heart. In fact, blood from the right side could easily travel to the left, causing low-oxygen blood to be pumped directly to the body. When this happens, cyanosis can occur. Auscultation of the murmur would also find it diminished or softer, compared to one without PVR.
PVR (or PVD, Pulmonary Vascular Disease as it is sometimes called) has a higher incidence in the Down Syndrome population. Children with this condition tend to develop and grow better than those without; however its presence tends to facilitate the repair of the AVSD sooner as there is a concern of the vessels becoming restricted permanently. Repairing the AVSD would lower the pressure in the pulmonary artery and therefore relieve the PVR.
The symptoms associated with a partial or intermediate AVSD tend to be more subtle than those of the complete AVSD. There is still an larger volume of blood being pumped through the pulmonary artery, however, the shunting effect takes place mainly in the atria, causing the pressure in the artery to remain slightly lower despite the larger amounts of blood being moved. The lower pressure causes causes less growth and breathing problems than experienced with a complete AVSD. The symptoms can be so subtle in fact, that a partial AVSD can remain undiagnosed for months and even years.
AVSD Treatment and Interventions
Occasionally this does not occur in an infant with a complete AVSD; instead a condition called Pulmonary Vascular Resistance (PVR) develops. In this, the smaller arteries of the lungs are constricted by the surrounding muscles to prevent them from being congested with the extra blood by the higher pressures of an AVSD. Due to this, many of the symptoms of congestive heart failure are prevented, including decreasing the amount of blood pushed (or "shunted") from the left to the right side of the heart. In fact, blood from the right side could easily travel to the left, causing low-oxygen blood to be pumped directly to the body. When this happens, cyanosis can occur. Auscultation of the murmur would also find it diminished or softer, compared to one without PVR.
PVR (or PVD, Pulmonary Vascular Disease as it is sometimes called) has a higher incidence in the Down Syndrome population. Children with this condition tend to develop and grow better than those without; however its presence tends to facilitate the repair of the AVSD sooner as there is a concern of the vessels becoming restricted permanently. Repairing the AVSD would lower the pressure in the pulmonary artery and therefore relieve the PVR.
The symptoms associated with a partial or intermediate AVSD tend to be more subtle than those of the complete AVSD. There is still an larger volume of blood being pumped through the pulmonary artery, however, the shunting effect takes place mainly in the atria, causing the pressure in the artery to remain slightly lower despite the larger amounts of blood being moved. The lower pressure causes causes less growth and breathing problems than experienced with a complete AVSD. The symptoms can be so subtle in fact, that a partial AVSD can remain undiagnosed for months and even years.
AVSD Treatment and Interventions
Initially, an AVSD may be treated with diuretics (such as Lasix) and ACE inhibitors (such as Ramipril) and antiarrhythmics (such as digoxin) to alleviate symptoms and give the patient some time to stabilize and/or grow before surgery.
Although some rare instances do close on their own, the vast majority of AVSDs require some form of surgical intervention (that varies, depending on the type and structures involved). Most often, complete AVSDs are repaired between 3-6 months of age and partial/intermediate taking place between 6-18 months. Once again, the severity, placement and structures involved dictate the precise procedure. Smaller "holes" may just require closing, where larger areas need to be "patched". Although this used to mean hospital stays of weeks at a time, most children are discharged home within just over a week of their surgery (the stay for complete AVSD repair is longer as it is more involved).
The survival rate for AVSD is also dependent on type, however all range between a 97-99% success rate. Follow up surgery may be required years later to tune up leaky valves (specifically the mitral valve). Anticoagulants may be prescribed if the valves become too leaky to prevent blood clots from forming. In the event that the electrical conduction of the heart becomes damaged, a pacemaker may have to be surgically installed. Later in life, a condition known as Sub-Aortic Stenosis can occur, where a blockage forms below the aortic valve and requires surgery to repair. Endocarditis can develop and any invasive procedures (such as dental cleanings, surgery, piercing and tattooing) will require antibiotics prior to prevent large amounts of bacteria from entering the bloodstream.
In Conclusion...
The diagnosis of an AVSD is no longer a death sentence. With recent advances in medicine, the management and repair of AVSDs has become almost routine. Although it remains a significant life event for you and your family, your child's diagnosis need not overwhelm every aspect of daily life. The vast majority of people (regardless of chromosome count) that have an AVSD repaired, go on to live happy, healthy, productive lives. It is difficult to learn that your child has a genetic disorder, of this I can attest first hand. Hearing that your child has issues with his or her heart can be even more frightening. However, with a little education and insight, this aspect of your child's health need not be devastating to you or your way of life.
---------------------------------
*Animations courtesy of Children's Heart Federation, ©2012.
Atrioventricular Septal Defect (AVSD), Children's Heart Federation, London, UK. 2012
Golding, Fraser, MD, Atrioventricular Septal Defect (AVSD), AboutKidsHealth, 2009
Hia, Cindy, MD, AVSD - Partially or Completely Confused?, The Children's Medical Institute, National University Hospital , Singapore
Horenstein, M Silvana, MD, Atrioventricular Septal Defect, Partial and Intermediate Clinical Presentation, Medscape Reference, 2012
Horenstein, M Silvana, MD, Atrioventricular Septal Defect, Partial and Intermediate Clinical Presentation, Medscape Reference, 2012




Wow...well done you, mama. So clear and concise, easy to read--and while it's technical you still managed to convey the warmth and positivity you are famous for. Thanks for this, it's going in my files for future reference and referral!
ReplyDeleteThanks so much. It's a bit dry, but I think all medical narritives are unless you are very interested in them. I'm glad you find it useful!
DeleteI have a granddaughter with Down Syndrome and AV Canal heart defect. She had her first surgery at barely 4 months old. She will be 9 yrs old in August. She just had her annual cardiologist appointment in April and we learned that her leakage had increased 11% from last year, she is now at 49% leakage which means another surgery soon. She has another appointment in August to see if the leakage has increased.
ReplyDeleteI am with you on ASVD is no longer a death sentence......We have a happy, joyful, almost nine year old little girl to prove that. :0)
Excellent Sharing !! I read your Posting, i like this.keep it up.Thanks a lot...
ReplyDeleteThank you very much!
DeleteMy 4 year old has a repaired AVSD. We has a stressful half year from when we found out at 8 months till 16 months when he had his surgery. He had trouble gaining wait as a baby and was catching every single virus. Thank g-d ever since his surgery he is a different child. He is healthy and energetic. Goes for checkup 2x a year. And he rarely gets sick. Last time a virus went through my family he was the only one who did not get sick
ReplyDelete:) So glad to hear it. Thanks for sharing your story.
DeleteThank you. I have a 3 month old daughter and she is schedule for surgery at 6 mos. I am scared for that day but I also want to get it over with. It's so Hard seeing her struggle to breath and eat. We have faith that it will all go well. And it's good to hear some of the great results after the surgery. If anyone has any advise on what to do, between now and the surgery, that will be helpful. Thanks everyone.
ReplyDeleteHow did the surgery go? Would like to follow up. :)
DeleteThanks for the comment and all the best for you and your family.